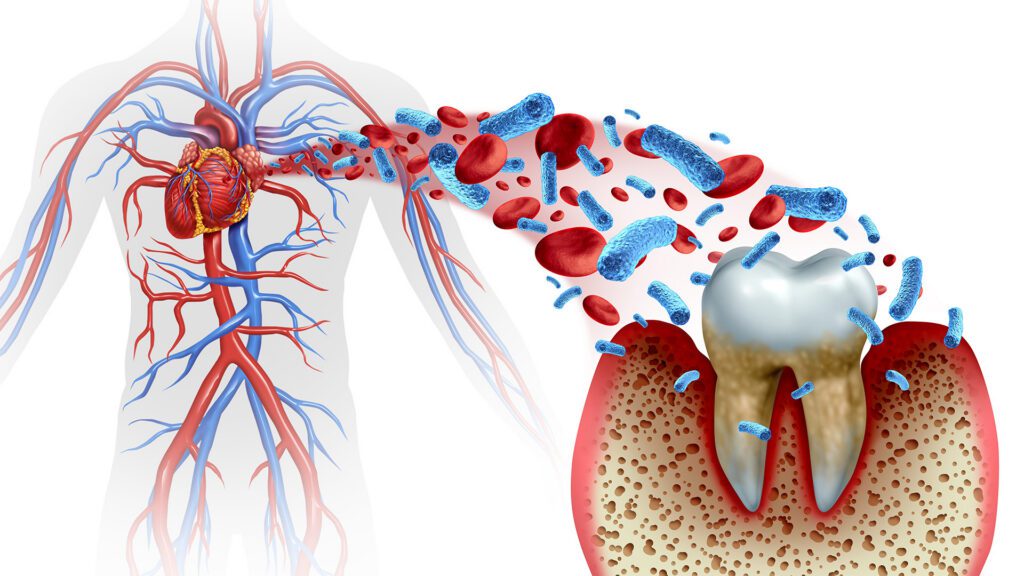
Many people are surprised to learn that gum health and blood sugar control are closely connected. Research has shown a strong, two-way relationship between periodontal (gum) disease and diabetes, meaning each condition can worsen the other if left untreated.
Understanding this connection is an important step toward protecting both your oral health and overall health.
What Is Periodontal Disease?
Periodontal disease is a chronic inflammatory condition that affects the gums and the bone supporting the teeth. It begins as gingivitis (gum inflammation) and can progress to periodontitis, where bone loss, gum recession, and even tooth loss can occur.
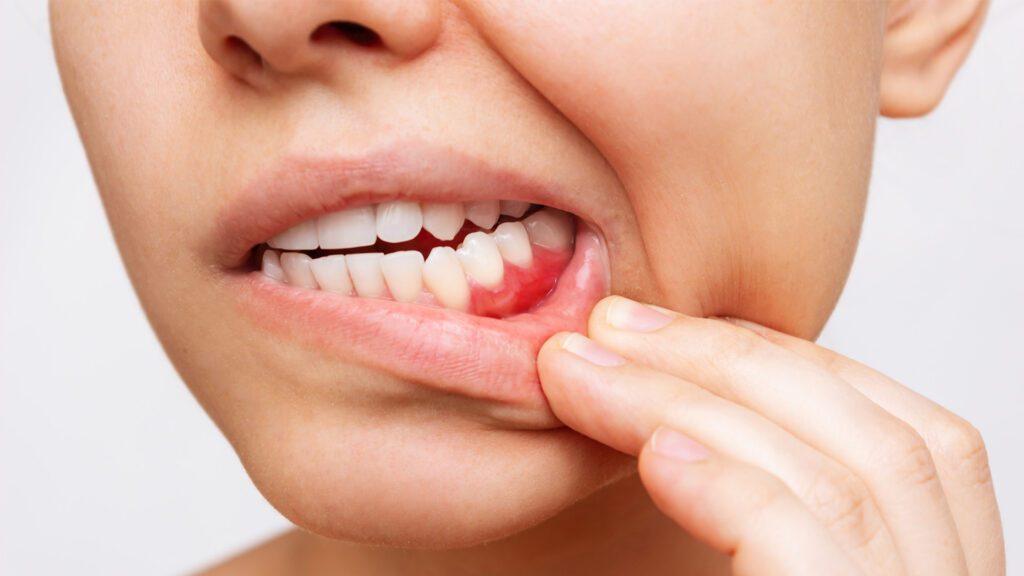
Common signs include:
- Bleeding gums
- Persistent bad breath
- Gum recession
- Loose teeth
- Tender or swollen gums
How Diabetes Affects Gum Health?
People with diabetes are more prone to infections, including gum infections. Elevated blood sugar levels can:
- Weaken the immune system
- Reduce the body’s ability to fight bacteria
- Slow healing after dental procedures
- Increase inflammation throughout the body
As a result, patients with diabetes are more likely to develop periodontal disease, and the disease may progress more rapidly.
How Periodontal Disease Affects Diabetes?
The relationship doesn’t go only one way. Active gum disease increases inflammation in the body, which can make it harder to control blood sugar levels.
Chronic inflammation from periodontal disease can:
- Increase insulin resistance
- Lead to higher A1C levels
- Make diabetes management more challenging
Studies have shown that treating periodontal disease can help improve blood sugar control in many patients with diabetes.
Why This Two-Way Relationship Matters?
When diabetes and periodontal disease coexist, they can create a cycle of worsening health:
- Poor blood sugar control increases gum inflammation
- Gum disease increases systemic inflammation
- Inflammation makes diabetes harder to manage
Breaking this cycle requires both medical and dental care working together.
What Patients with Diabetes Should Do?
If you have diabetes, protecting your gums is essential. Recommendations include:
- Regular periodontal evaluations
- Professional cleanings at appropriate intervals
- Early treatment of gum inflammation
- Excellent home oral hygiene
- Collaboration between your dentist, periodontist, and physician
Early detection and treatment can prevent bone loss, tooth loss, and complications that affect overall health.
How a Periodontist Can Help?
A periodontist specializes in treating diseases of the gums and bone. Treatment options may include:
- Deep cleaning (scaling and root planing)
- Laser periodontal therapy
- Periodontal maintenance
- Regenerative procedures when bone loss is present
These treatments aim to reduce inflammation, control infection, and preserve the structures that support your teeth.
Healthy Gums Support a Healthier Body
Periodontal health is not just about your smile — it plays a role in your long-term systemic health. For patients with diabetes, maintaining healthy gums is an important part of comprehensive care.
If you have diabetes and are experiencing bleeding gums, gum recession, or loose teeth, a periodontal evaluation may be an important next step.
Schedule a Periodontal Evaluation
Brier Creek Implants & Periodontics
(919) 278-7298
www.briercreekimplantsandperio.com
Specialized care focused on gum health, bone preservation, and long-term stability.